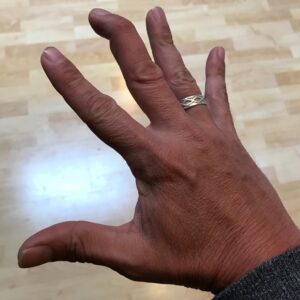
MALLET FINGER
If you suffer from pain in the affected joint or deformity, please Schedule an appointment with one of our orthopedic specialists as soon as possible.
What is Mallet Finger?
Mallet finger occurs when an event injures the tendon that straightens the end of a finger. Also colloquially known as “baseball finger,” Mallet finger can still happen to anyone when an object (such as a ball) forcefully impacts the tip of their finger or thumb and bends the digit further than they can go.
Following the injury, patients will lose the ability t0 straighten the tip of their finger or thumb on their own. Moreover, the 3rd, 4th and 5th fingers of the dominant hand have the highest risk of this injury. Additionally, the finger commonly feels painful, swollen, and bruised. Moreover, the tip of the finger will have noticeably drooped and will only straighten if pushed. Untreated Mallet Finger can lead to a Swan Neck Deformity.
What Causes Mallet Finger?
Sudden flexion of the distal interphalangeal (DIP) joint with resistance force directed along the long axis of the finger remains the most commonly known mechanism of injury. Furthermore, this sudden flexion and resistance causes avulsion of the tendon with a bony fragment or tear in the terminal extensor.
Common among athletes, a forceful blow to the tip of the finger causing sudden flexion remains the common cause. Baseball players often present with the diagnosis of a “jammed” finger. Laceration, deep abrasions, or crashes result in open injuries. Mallet finger secondary to a dorsal lip fracture may result from DIP joint hyperextension when the hyperextended distal phalanx impacts on the head of the middle phalanx (Alla, Deal and Dempsey, 2014).
Who is at Risk of Mallet Finger?
Experts say young and middle-aged males report more with this condition than other age groups and females. Additionally, most cases come from sports or work-related activities. Reports made on an incidence of mallet finger in a familial distribution suggest the involvement of a genetic disposition that makes individuals susceptible to sustaining mallet finger injuries. The majority of mallet fingers present as closed injuries while a few, resulting from lacerations in the dorsal aspect of the distal phalanx or crash injuries present as open injuries (Lamaris and Matthew, 2016).
How is Mallet Finger Diagnosed?
Treatment Options for Mallet Finger
Non-operative management remains the main treatment option for nearly all mallet finger injuries. For injuries with no volar subluxation of the distal phalanx, no associated fracture, or cases with less than one-third of the articular surface involved, non-operative management gets utilized. Non-operative treatment involves total immobilization of the associated joint in full extension or slight overextension for at least 6 weeks, followed by 2 weeks of nighttime splinting. Continuous and complete immobilization of the affected joint must happen so that the distal interphalangeal joint does not flex.
Experts recommend that when the distal interphalangeal joint flexes during the course of 6 weeks, the course needs a restart. Several types of splint have proven useful for maintaining the distal interphalangeal joint in extension and subsequently the ruptured extensor tendon in apposition. When patients respond poorly to continuous splinting or in cases of certain professionals, such as surgeons and musicians, surgery may save the day (Lamaris and Matthew, 2016).
Please do not hesitate to contact us if you have any questions.
References
Alla, S.R., Deal, N.D. and Dempsey, I.J. (2014). Current Concepts: Mallet Finger. HAND, 9(2), pp.138–144.
Lamaris, G.A. and Matthew, M.K. (2016). The Diagnosis and Management of Mallet Finger Injuries. HAND, [online] 12(3), pp.223–228. Available at: https://pubmed.ncbi.nlm.nih.gov/28453357/ [Accessed 11 Feb. 2022].
Lin, J.S. and Samora, J.B. (2018). Surgical and Nonsurgical Management of Mallet Finger: A Systematic Review. The Journal of Hand Surgery, [online] 43(2), pp.146-163.e2. Available at: https://pubmed.ncbi.nlm.nih.gov/29174096/ [Accessed 11 Feb. 2022].