RAYNAUD’S DISEASE
If you suffer from Raynaud’s disease, please Schedule an appointment with one of our orthopedic specialists as soon as possible.
What is Raynaud’s Disease?
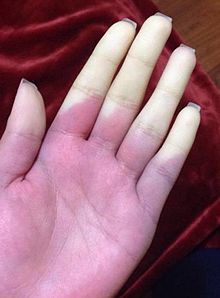 Raynaud’s Disease (also called Raynaud’s Syndrome or Raynaud’s Phenomenon) causes decreased blood flow to the fingers. In some patients it may also cause reduced blood flow to the knees, ears, toes, or nose. This occurs due to spasms in the blood vessels of those areas. The spasms can trigger in response to cold, stress, or emotional turmoil.
Raynaud’s Disease (also called Raynaud’s Syndrome or Raynaud’s Phenomenon) causes decreased blood flow to the fingers. In some patients it may also cause reduced blood flow to the knees, ears, toes, or nose. This occurs due to spasms in the blood vessels of those areas. The spasms can trigger in response to cold, stress, or emotional turmoil.
Raynaud’s can occur by itself (Primary Form), or it may occur alongside other diseases (Secondary Forms). The diseases most often linked with Raynaud’s include:
- Lupus (systemic lupus erythematosus)
- Scleroderma
- CREST syndrome (a form of scleroderma)
- Buerger disease
- Sjögren syndrome
- Rheumatoid arthritis
- Occlusive vascular disease
- Polymyositis
- Blood disorders, such as Cryoglobulinemia
- Thyroid disorders
- Pulmonary hypertension
The primary form of Raynaud’s Syndrome occurs the most commonly. It often presents between the ages of 15 and 25. People with primary Raynaud’s usually do not develop a related condition, and experience less severe symptoms than secondary Raynaud’s.
What Causes Raynaud’s Disease?
Doctors do not know the exact cause of Raynaud’s Disease. Theories suggest that some blood disorders increase blood thickness, due to excess platelets or red blood cells. Special receptors in the blood that control the narrowing of the blood vessels may also lie at the root of Raynaud’s Disease.
Who is at Risk For Raynaud’s Disease?
Risk factors that can increase the probability of developing Raynaud’s Disease include:
- An Autoimmune Disease
- Chemical Exposure
- Smoking Cigarettes
- Injury or Trauma
- Repetitive Actions such as typing or use of vibrating tools such as a jackhammer
- Side effects of certain medicines
What are the Symptoms of Raynaud’s Disease?
Symptoms can appear differently depending on the patient. Common symptoms may include:
- Fingers turning pale or white and then blue when exposed to cold, stress or emotional turmoil, then back to red when warm again.
- Hands swell painfully when warm.
- Sores developing on the finger pads.
- Gangrene that causes infection in the fingers that may require amputation in rare cases.
How is Raynaud’s Disease Diagnosed?
During a physical exam, a physician may expose a patient’s hand to a cold challenge test, and watch to see how the color changes in the hands and fingers. Physicians may also use a microscope to examine the small blood vessels in the fingernails. Adults who develop Raynaud’s Disease after the age of 35 may need further testing for underlying diseases. Patients may also have blood tests done to see if they have primary or secondary Raynaud’s.
How is Raynaud’s Disease Treated?
Treatment depends on the symptoms, age, and general health of the patient. It also depends on the severity of the condition. While Raynaud’s Disease lacks a cure, patients can manage it by taking proper steps. Treatment may include:
- Avoid the cold
- Wear warm clothing items such as gloves
- Stop smoking
- Wear guards over fingers with sores
- Avoid trauma or using vibrating tools
- Take blood pressure medication during the winter months to help reduce blood vessel constriction.
What are the Complications of Raynaud’s Disease?
In rare cases, the finger pads may produce sores that progress to gangrene. In rare cases, gangrene can lead to amputation of the affected finger.
Living with Raynaud’s Disease
For most patients diagnosed with Raynaud’s Disease, they find it more of an inconvenience than a problem. Patients careful to avoid triggers, such as the cold, can reduce the frequency of symptoms. If patients suffer from an underlying cause, such as lupus, they may find it more difficult to manage Raynaud’s symptoms. Patients with secondary Raynaud’s should work together with their healthcare provider to manage their conditions to decrease attacks of Raynaud’s.
If you would like to speak to an Orthopedic Upper Extremity Specialist in North Texas, give us a call at 817-697-4038, or contact us over the web. Tele-medicine appointments are also available.

