TRIGGER FINGER
If you suffer from severe pain caused by trigger finger, please Schedule an appointment with one of our orthopedic specialists as soon as possible.
WHAT IS TRIGGER FINGER?
 Hand and wrist specialists define this condition as a condition in which one or more fingers has trouble flexing and extending. Additionally, the finger may experience a ‘pop’ as it bends down or straightens, and can even be unable to bend all the way down or be unable to straighten without help from the other hand. Moreover, any of the fingers including the thumb can suffer from Trigger Finger, and it can affect multiple fingers at once.
Hand and wrist specialists define this condition as a condition in which one or more fingers has trouble flexing and extending. Additionally, the finger may experience a ‘pop’ as it bends down or straightens, and can even be unable to bend all the way down or be unable to straighten without help from the other hand. Moreover, any of the fingers including the thumb can suffer from Trigger Finger, and it can affect multiple fingers at once.
The medical term for this condtion, ‘stenosing tenosynovitis’, means an inflammation of the fluid surrounding the flexor tendon, or tenosynovium, and this results in compression of the tendon which interferes with its gliding function. Furthermore, this condition has a 2-3% lifetime risk of developing in patients, and 10% lifetime risk in diabetics.1,2
WHAT CAUSES TRIGGER FINGER?
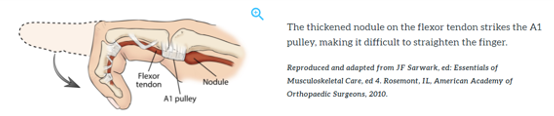
Flexor tendons in the fingers run through tunnels of connective tissue known as ‘pulleys’. However, there are many pulleys in the finger, but the first one, also known as the A1 pulley has the highest risk of causing this condition. Moreover, this condition occurs when the pulley becomes too tight for the tendon to fit through due to inflammation of the tendon, the surrounding tenosynovium, or the A1 pulley. Additionally, instead of easily gliding through the tunnel, the flexor tendon will have difficulty moving or will not move at all.
Risk factors for developing this condition include: female sex, diabetes, rheumatoid arthritis, activities which include repetitive gripping and finger flexion.
WHAT ARE THE SYMPTOMS OF TRIGGER FINGER?
Signs and symptoms include:
- Waking up with a flexed finger that pops when it is straightened.
- A popping or clicking feeling when moving the finger.
- Tenderness or a small bump at the base of the affected finger.
- Can present with inability to flex the finger all the way down, or inability to extend the finger all the way.
DIAGNOSIS AND TREATMENT OF TRIGGER FINGER
DIAGNOSIS OF TRIGGER FINGER
Moreover, Hand and Wrist Specialists diagnose this condition following a clinical evaluation and examination. Additionally, history consistent with finger triggering and recreation of finger locking or triggering on physical examination confirms the diagnosis.
TREATMENT OF TRIGGER FINGER
The treatment ranges from non-operative to operative:
- Lifestyle modifications: such as resting the hand and decreasing repetitive gripping activities and wearing a splint to keep the finger extended at night may improve mild symptoms.
- NSAID medications: can act to decrease inflammation in the tendon and A1 pulley to increase gliding of the tendon.
- Hand therapy: exercises can help work on tendon gliding and decreasing edema.
- Steroid injection: performed over the A1 pulley in the office. Studies show that 66% of this condition resolve after one injection, with trigger thumbs having higher resolution rates than the other fingers.4
- Surgical release: Surgeons make a small incision in the palm close to the base of the affected finger and divide the A1 pulley. This allows the flexor tendons to glide without inhibition.
If you would like to speak to an Orthopedic upper extremity Specialist in North Texas, give us a call at 817-697-4038, or contact us over the web. Tele-medicine appointments are also available.
FURTHER READING
AAOS – American Academy of Orthopaedic Surgeons trigger finger OrthoInfo webpage. https://orthoinfo.aaos.org/en/diseases–conditions/trigger-finger/
ASSH- American Society of Hand Surgery trigger finger Handcare webpage. https://www.assh.org/handcare/condition/trigger-finger
REFERENCES
- “Trigger finger in diabetes” by Strom published in Journal of Medical Society in 1977. https://pubmed.ncbi.nlm.nih.gov/269967/
- “Outcome of trigger finger treatment in diabetes” by Stahl et al published in the Journal of Diabetes Complications in 1997. https://pubmed.ncbi.nlm.nih.gov/9334911/
- “Essentials of musculoskeletal care” by Sarwark et al published by the American Academy of Orthopaedic Surgeons in 2010.
- “The efficacy of steroid injection in the treatment of trigger finger” by Dala-Ali et al published in Clinics in Orthopedic Surgery Dec 2012. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3504690/

